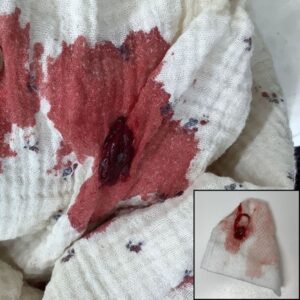
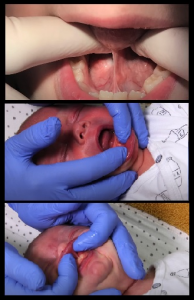
Other things you may notice after the release
After the release, you may notice things that may last a little longer, such as lip swelling, drooling, gagging, or other discomfort or peculiarities.
* Granulation tissue; This is a small lump of extra scar tissue that can form on the wound. If you suspect you see this, send a photo, it is not serious and if it is a hindrance to drinking it can still be removed.
* Drooling; Because the swallow has to be learned again after tongue tie release, it is possible to notice drooling for a while in a child or baby.
* Reattachment; After the treatment, the wound simply wants to heal with scar tissue. With doing aftercare you hope the wound does not close too quickly or too tightly. If too much reattachment occurs, the tongue or lip mobility can be limited again. When you live abroad it is the adviceble to check the healing with somebody knowledgable in a week, that can also be done at our clinic if you can stay a few days, but has to be arranged with making the appointment for treatment. In The Netherlands you can call the Tongue Tie Clinic for an appointment.
* Muscle pain; After the treatment the adults and older children notice (muscle) pain or discomfort in the jaws, tongue and throat sometimes as well. See the FAQ about pain relief.
* Baby spits more; Because the baby drinks more effectively, it may be that the stomach is not used to the amounts and it spits back up, but it may also be that the baby is still drinking air for a while.
* Smelly breath / mouth; We sometimes hear this from parents and can last from a few days to a week, it’s ussualy no problem whatsoever.
* Swollen upper lip; This can last for up to 5 days after lipband treatment.
* Quivering jaws remain visible longer; Because the tongue, after it has come loose, many of the muscles still need to be trained, it may be that the compensation continues with the jaw muscles, but compensation behavior may also need a chiropractor or manual therapist to remedy it. See the FAQ about compensation behavior and videos explaining this.
* You have to help lips flange out; The baby is not used to flanging the lip, this may be helped.
* Suction blisters still present; They can be present for longer, especially on the upper lip.
* Crying doing aftercare; What we hear from parents and notice at the aftercare consultation that the baby cries with the aftercare exercises, but stops as soon as you stop or start feeding or changing diaper and such.
* White plaques/debris on tongue still visible; Because the palate is often high and the tongue is not well trained to stay up, even at rest, the white plaques/ debris on the taste buds remains.
* Bottleteat; We notice that the teats with a broad base cannot go deeper into the mouth, so a teat that can go deeper and gives more mouthfilling, such as the smaller, narrower types, is often better.
* Baby stays upset longer than 48 hours, crying, drinking worse. In the older baby who has had to compensate for a long time with a tongue tie. Before the treatment, often these babies were fussy and drinking poorly and found there own “technique”. Treatment of compensation behavior is often necessary. See FAQ compensation behavior. People often give painkillers for longer. But one also has to take into account a normal virus infection occurs at the same time. You can go to the doctor with a fever, see the FAQ about fever.
* Gagging may still be present after the release.
* A baby cannot swallow the tongue after the release.
* Apnea are also observed in babies . It is not directly related to the release. Tongue tie can be related, read the research.